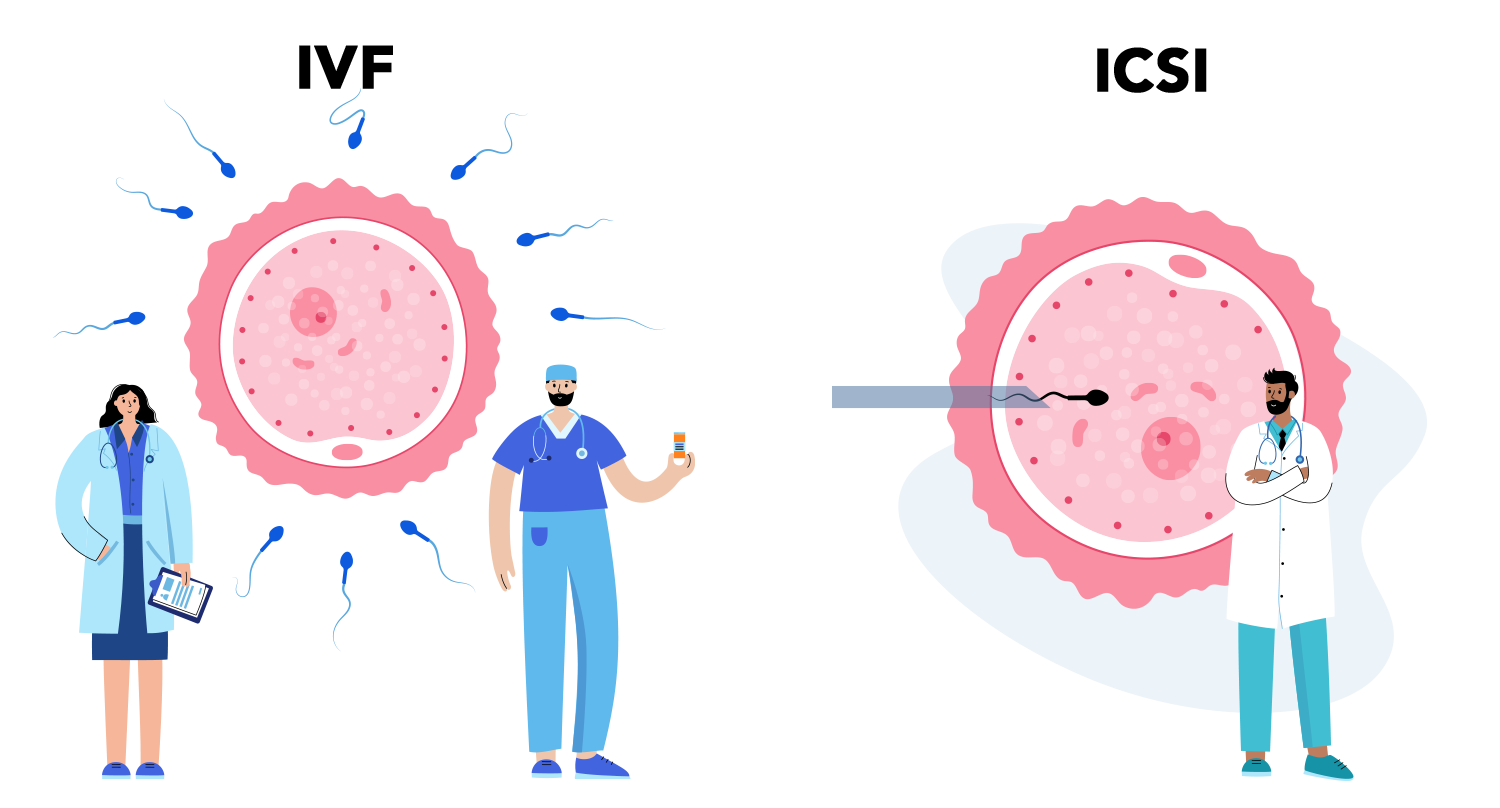
Intracytoplasmic Sperm Injection (ICSI) and Physiological Intracytoplasmic Sperm Injection (PICSI) are both advanced techniques used in assisted reproductive technology (ART) to help couples struggling with infertility. These methods focus on enhancing the chances of successful fertilization bydirectly injecting a single sperm into an egg, which helps overcome male factor infertility.Although ICSI and PICSI share certain similarities, they have notable differences that make each technique suitable for specific situations. Below, we’ll break down the similarities, differences, and unique advantages of ICSI and PICSI, making it accessible to both professionals and laypeople.
Similarities Between ICSI and PICSI
Purpose: Both ICSI and PICSI are designed to address male infertility problems, particularly when the male partner has issues such as low sperm count, poor motility, or abnormal sperm shape. Both techniques can be used for couples with a history of unsuccessful fertilization during conventional in vitro fertilization (IVF).
Procedure: In both ICSI and PICSI, a single sperm is selected and directly injected into the egg. This bypasses the natural process of the sperm having to swim through and penetrate the egg, which can be helpful when sperm quality is compromised.
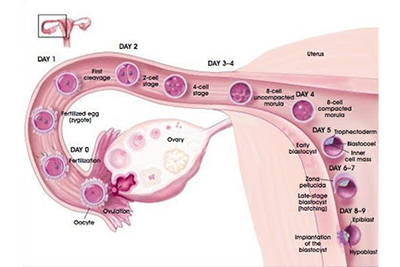
IVF Treatment:ICSI and PICSI are steps within the broader process of IVF, typically performed after the eggs are retrieved from the female partner.
Laboratory Setting:Both procedures are performed in a highly controlled laboratory setting, under the microscope, by skilled embryologists.
Differences Between ICSI and PICSI
Sperm Selection Method:
- ICSI: During ICSI, the embryologist manually selects a sperm based on its appearance, such as its motility and shape. This selection is largely subjective and relies on the experience of the embryologist to identify healthy sperms.
- PICSI: PICSI takes a more physiological approach to sperm selection. It involves using a specialized dish that contains hyaluronic acid, a substance found naturally in the egg’s outer layer. Only mature and healthy sperm are capable of binding to this substance. By
selecting sperm that can bind to hyaluronic acid, the PICSI process aims to mimic the natural selection that would occur in the body, potentially resulting in better fertilization outcomes.
Physiological Advantage:
- ICSI: In ICSI, sperms are selected based on observable characteristics, which may not always guarantee their genetic quality. The embryologist’s expertise plays a key role in ensuring that only viable-looking sperm are used.
- PICSI: In contrast, PICSI helps select sperm that are biochemically mature and capable of binding to hyaluronic acid, which isbelievedto correlate with lower rates of chromosomal abnormalities and better fertilization potential.
Why Choose ICSI?
ICSI is widely used in ART, especially when dealing with severe male factor infertility. Here are the main reasons why ICSI may be the preferred choice:
- Severe Male Infertility:When the sperm count is extremely low or sperm motility is poor, ICSI allows direct injection of sperm into the egg, overcoming the barriers posed by natural fertilization.
- Egg Penetration Issues: Some couples may have had unsuccessful IVF cycles where sperm failed to penetrate the egg. ICSI ensures the egg is fertilized by directly injecting the sperm.
- Use of Frozen Sperm: ICSI is particularly useful when working with sperm that has been frozen, such as in cases where the male partner has undergone cancer treatment or in cases of preserved fertility.
- Unexplained Infertility:For couples facing unexplained infertility, ICSI can improve the chances of fertilization by manually facilitating the process.
- Previous IVF Failures:If previous IVF attempts have failed due to poor fertilization, ICSI can be used to directly assist in fertilizing the egg, bypassing potential problems in natural sperm- egg interaction.
- Surgically Retrieved Sperm:Incases of obstructive azoospermia, fertilization is made possible through ICSI after the sperms have been surgically retrieved from the testes.
Why Choose PICSI?
PICSI can be advantageous in specific scenarios where sperm quality and maturity are critical. Here are reasons why PICSI may be selected:
- Sperm Quality Concerns:When sperm DNA fragmentation is suspected to be a cause of infertility or recurrent miscarriage, PICSI can help in selecting mature sperm with better genetic integrity.
- Recurrent IVF Failures: In cases where standard ICSI has not led to successful pregnancy despite good egg quality, PICSI may help in achieving better outcomes by selecting biochemically mature sperm.
- Improved Embryo Quality:Since PICSI involves using sperm that can bind to hyaluronic acid, it may lead to improved embryo quality, which in turn can result in higher pregnancy rates and better outcomes for the couple.
Advantages of ICSI
Reliable and Established:ICSI has been used in IVF for decades and has proven to be highly effective, especially in male factor infertility cases.
Works with Limited Sperm:Even if there are very few sperm, ICSI can still achieve fertilization, making it suitable for men with obstructive azoospermia after surgical sperm retrieval procedures.
Advantages of PICSI
Mimics Natural Selection: PICSI adds an additional layer of selection by mimicking the natural sperm selection process, which may lead to healthier embryos and better implantation rates.
Potentially Fewer Miscarriages: By selecting mature sperm with lower DNA fragmentation, PICSI may help reduce the rate of miscarriage compared to traditional ICSI.
Conclusion
ICSI and PICSI are valuable tools in the realm of assisted reproductive technology, each with unique strengths. ICSI is the standard procedure for overcoming male infertility, allowing fertilization to occur even with a low number of sperm. PICSI takes an extra step by selecting more mature and genetically competent sperm, potentially leading to better outcomes, especially for couples experiencing recurrent IVF failures or miscarriages.
For couples considering assisted reproductive technology, the choice between ICSI and PICSI will depend on individual circumstances, particularly the male partner’s sperm quality and any prior experiences with IVF. Consultation with a fertility specialist is key to determining which procedure will provide the best chance of achieving a successful pregnancy.